When practitioners disagree
In this sub-section
- Introduction (this page)
- Caffeine for breathing problems in premature babies
- Antibiotics in pre-term labour
- Breast cancer
Introduction
For many diseases and conditions, there is substantial uncertainty about the extent to which treatments work, or about which treatment is best for which patient. That doesn’t stop some doctors having very strong opinions about treatments, even though those opinions may differ from one doctor to the next. This can lead to considerable variation in the treatments prescribed for a given condition.
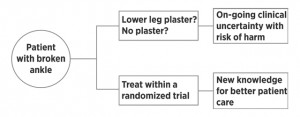
In the 1990s, Iain Chalmers, one of the authors, while holidaying in the USA, broke an ankle and was treated by an orthopaedic surgeon. The surgeon put the leg in a temporary splint, and said that the next step, once the swelling had subsided, would be a lower leg plaster cast for six weeks. On returning home a couple of days later, Iain went to the local fracture clinic, where a British orthopaedic surgeon, without hesitation, dismissed this advice. Putting the leg in plaster, the British surgeon said, would be wholly inappropriate. In the light of this obvious professional uncertainty, Iain asked whether he could participate in a controlled comparison to find out which treatment was better. The British surgeon answered that controlled trials are for people who are uncertain whether or not they are right – and that he was certain that he was right.
How can such a pronounced difference in professional opinion come about, and what is a patient to make of this? Each surgeon was certain, individually, about the correct course of action. Yet their widely divergent views clearly revealed uncertainty within the profession as a whole about the best way to treat a common fracture. Was there good evidence about which treatment was better? If so, was one or neither surgeon aware of the evidence? Or was it that nobody knew which treatment was better (see Figure).
Facing up to uncertainties: a matter of life and death
“Failure to face up to uncertainties about the effects of treatments can result in avoidable suffering and death on a massive scale.”
There are several separate issues here. First, was there any reliable evidence comparing the two very different approaches being recommended? If so, did the evidence show their relative effects on outcomes (reduced pain, or reduced muscle wasting, for example) that might matter to Iain or to other patients, who might have different preferences to his? But what if there was no evidence providing the information needed?
Some clinicians are clear about what to do when there is no reliable evidence about the effects of alternative treatments and are prepared to discuss this uncertainty with patients. For example, one doctor who specializes in caring for people with stroke, commented that, although research evidence shows that his patients would fare better if cared for in a stroke unit, it remained uncertain – for many types of patients – whether they should receive clot-busting drugs.
Addressing uncertainty is professional
“One of the key attributes of professionalism … should be the ability to identify and address uncertainty in medicine.”